Doctors and nurses taking care of patients suffering from COVID-19 are at particular risk of picking up the infection themselves. A collaboration between an engineer and a medical specialist might keep them safe.
Early this past March, when vast numbers of Australians were just beginning to consider what reports of a new coronavirus might mean for our lives, Dr Forbes McGain was already thinking about how bad the impending pandemic could get.
So McGain, an intensive care specialist at Western Health, phoned up some contacts at the University of Melbourne, who put him in touch with Professor Jason Monty.
“He called us and said he was really concerned about infection in healthcare workers due to this terrible pandemic,” Monty told create.
Monty thought he could help, even though, as head of mechanical engineering at Melbourne, he had never previously worked in healthcare.
His expertise is in fluid dynamics, and that turned out to be an ideal specialty for someone looking to contain the spread of the coronavirus.
“The biggest deal with this virus is that it travels on droplets,” Monty explained.
“Understanding how droplets will travel around the room is our expertise and we just didn’t know it was such a relevant problem to the pandemic until we were asked to do this.”
Negative pressure
The solution Monty and McGain came up with was a personal ventilation hood that could be placed over a bed in an intensive care unit, whisking away infectious fluid particles while still allowing medical workers to access their patients.
Usually, when a hospital needs to isolate someone to contain infections like this, it can place the patient in a negative pressure room — a space with a ventilation system that permits air to flow in but not escape other than through specially installed filters.
But most intensive care units only have one or two of these — enough for normal times, but unsuitable for a pandemic.
“You’re not going to be able to build a thousand of those anytime soon,” Monty said.
“They cost hundreds of thousands of dollars to make and take up valuable space.”
McGain saw another problem.
“The nurses in the negative pressure room looking after the patient are exposed to the disease,” he said.
Other countries with intensive COVID-19 outbreaks have solutions that tend to be unwieldy for both patients and medical staff — McGain calls a bubble device used in Italy to enclose a patient’s head a “diving hood”, while Monty compares a UK bed compartment to a coffin.
“You then can’t do lots of things in them,” McGain said.
“You certainly can’t eat, and you can’t really speak that well, and it is just a cumbersome and difficult thing to deal with.”
Another alarming problem Monty identified: if anything goes wrong with the ventilation system, the patient could asphyxiate before medical staff can fix the problem.
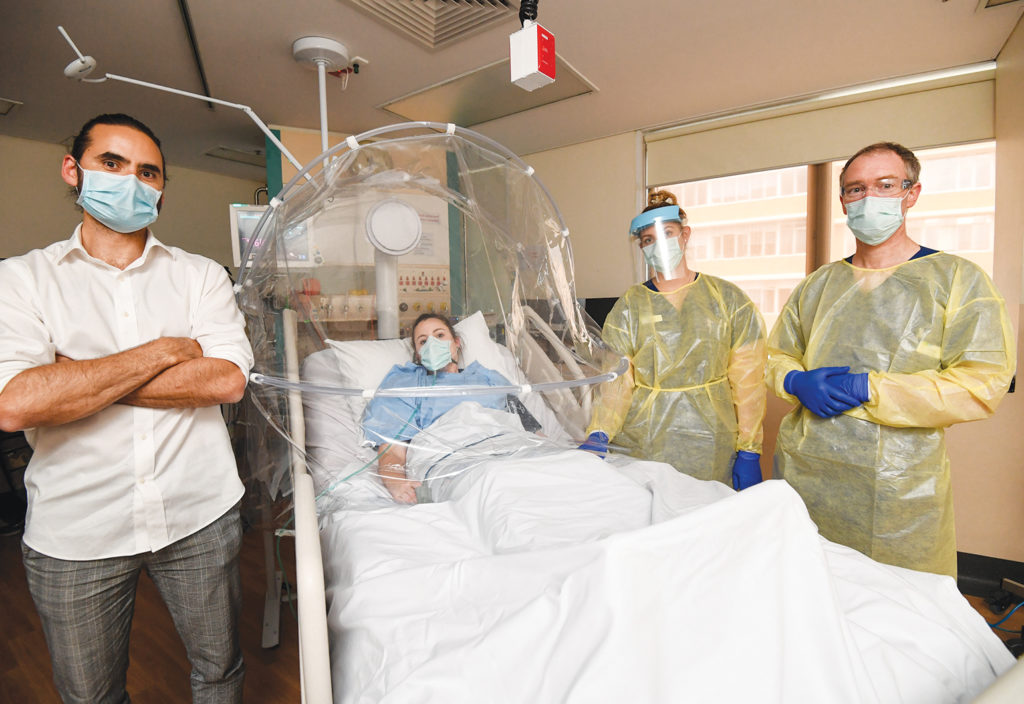
Monty and McGain’s hood solution, however, can be easily removed if it needs to be.
“Most important is its safety,” McGain said.
“Just open it up and push it backwards. If the patient is deteriorating, it just gets out of the way very quickly. That’s absolutely vital.”
Keep it simple
When Monty and McGain first started brainstorming a better solution, they lit upon a baby’s pram as a model for their device.
“We’re fluid dynamics researchers — my idea was why do you need to seal off the patient if you can just constantly draw air past them and there’s no risk of the infection getting to anyone nearby,” Monty said.
“It’s basically an articulated hood that can fold backwards and forwards and it’s made of clear plastic. When it drapes down over the patient, it covers the patient, roughly the head and torso, but not their whole body, and then the plastic from the hood just drapes down over the bed … allowing air to come up through the gaps between the hood and the bed.”
A ventilation system, which Monty compares to a range hood exhaust, sucks air from behind the patient’s head and extracts it through a high-efficiency particulate air filter that removes 99.97 per cent of particles.
One benefit of the device is its simplicity — which makes it cheap to produce and easy to deploy.
“As things become more complex, things go wrong or are more likely to,” McGain said.
“I think it’s great what the engineering team has come up with to make actually a very simple design that is mobile and safe and yet effective.”
In fact, it is so simple that the team built its first prototype out of materials picked up from Bunnings and Clark Rubber.
“Keeping costs down was extremely important to us in the beginning — not just to keep the cost down, but to make it something that you could easily and quickly produce,” Monty said.
“It turned out that the products that we used, which are all off-the-shelf components, only ended up costing about $600 and that’s at commercial costs. Literally buying it off the shelf.”
That was important, considering that they were gathering materials at a time when shops across the country were closing, supply chains were being interrupted, and even soap and toilet paper had vanished off the shelves — let alone specialist medical goods.
“We’re not using any of the kinds of materials that are used for other [personal protective equipment] that can’t be made, which was a real benefit,” Monty said.
Listening to the experts
Crucial to the design was the advice the team received from nurses as they tested their ideas.
“The intensive care nurses in particular have been very useful in giving advice,” McGain said.
“For example, when the first hood came out, it was just too small. When the second prototype came out, it didn’t quite have the right height of the sidebars.”
The nurses could recognise better than the engineers when certain design features would obstruct patient care.
Monty says the feedback from Western Health also helped the team understand what could make patients more comfortable.
“We learned very quickly how to build the thing and that we could get the components that we needed and that it would be effective,” he said.
“The big problem was, how do we know that this is going to be comfortable and usable for the nurse and for the patient?”

The next step is to conduct trials, which will take place at Victoria’s Footscray Hospital, and then meet the rigorous approvals process so that the device can be rolled out into hospitals across Australia — and the world.
“The World Bank has already contacted us to say that they would love to deploy this in Africa,” Monty said.
And even if the COVID-19 pandemic should be brought under control everywhere, McGain says the hood will remain useful.
“This can be used in the long term, in particular for people with [tuberculosis] or influenza, measles, all sorts of other pandemics,” he said.
“This is not something that’s going to go away. A pandemic is one of the most predictable things in the universe.”
Engineering during a pandemic
For Monty, one of the biggest uncertainties with working in a pandemic were issues around the supply chain. Would the parts he needed be available now — or in two weeks’ time? Would shops he needed to buy from still be open? Could he rely on deliveries to continue?
“We had no idea whether we would still be able to go to Bunnings from the 28th of March and buy a fan, or will an acrylic supplier still be open?,” he told create.
“We learned a lot about how business continues in a pandemic. There’s some businesses, some manufacturers, you think would stay open and are closed and you’d find some others that you think surely wouldn’t have any business and are able to continue and, in some cases, even thrive.”
Non-specialist vendors were able to build the components they needed — the team relied on a local flag and sign manufacturer and a fan supplier and manufacturer for the parts they needed.
The other difficulty with carrying on engineering work while the country was shutting down was that even being around other people carried inherent risks.
“It was a little nerve-wracking,” Monty said.
“We did our best to social distance, but we were trying to find a solution within a very short timeframe. It was difficult, and I did have to ask for consent, because I was asking people to be in a workplace that was shut down due to the health concerns.”



This negative system cannot guarantee the virus not sneaking out to the room. Obviously the room has to be under a negative pressure so much less chance of virus sneaking out of the room. The COVID-19 will live on human skin. Overall virus-tight suit has to be worn to completely isolate the doctor from any trace of this virus. Not just an apron which only covers the front. At least N95 mask has to be worn. The holes on N95 mask are actually larger than this virus. Full eye protection has to be worn since the virus can infect through eyes too. I am afraid the doctors may have to wear nappies to avoid going to toilet. Every time the suit is removed, either a new suit is required, or the same suit has to be sterilized and the person has to be very cautious not to touch any part of the outside of the suit and any other protection. And any disposal has to be treated carefully (it is ignored here in Australia unfortunately). All these steps are the routine practices in China to successfully keep the virus under control. They cannot be avoided until new better ways are found. Just a thought for future, if an inexpensive protective membrane, which can zap the virus, can be easily wrapped onto the surface of a person, remains effective for 2-3 hours and can be easily removed and it is also degradable.
After reading this I am more concerned it seems impossible to outwit this virus in our pride we think we can , hope we have a vaccination soon ,
This virus us not a living thing. It is a lifeless protein.