As one of the founders of biomedical company Seer, George Kenley is helping to revolutionise the treatment of epilepsy. However, before working to improve patients’ lives, this engineer had spent more than a decade on construction projects.
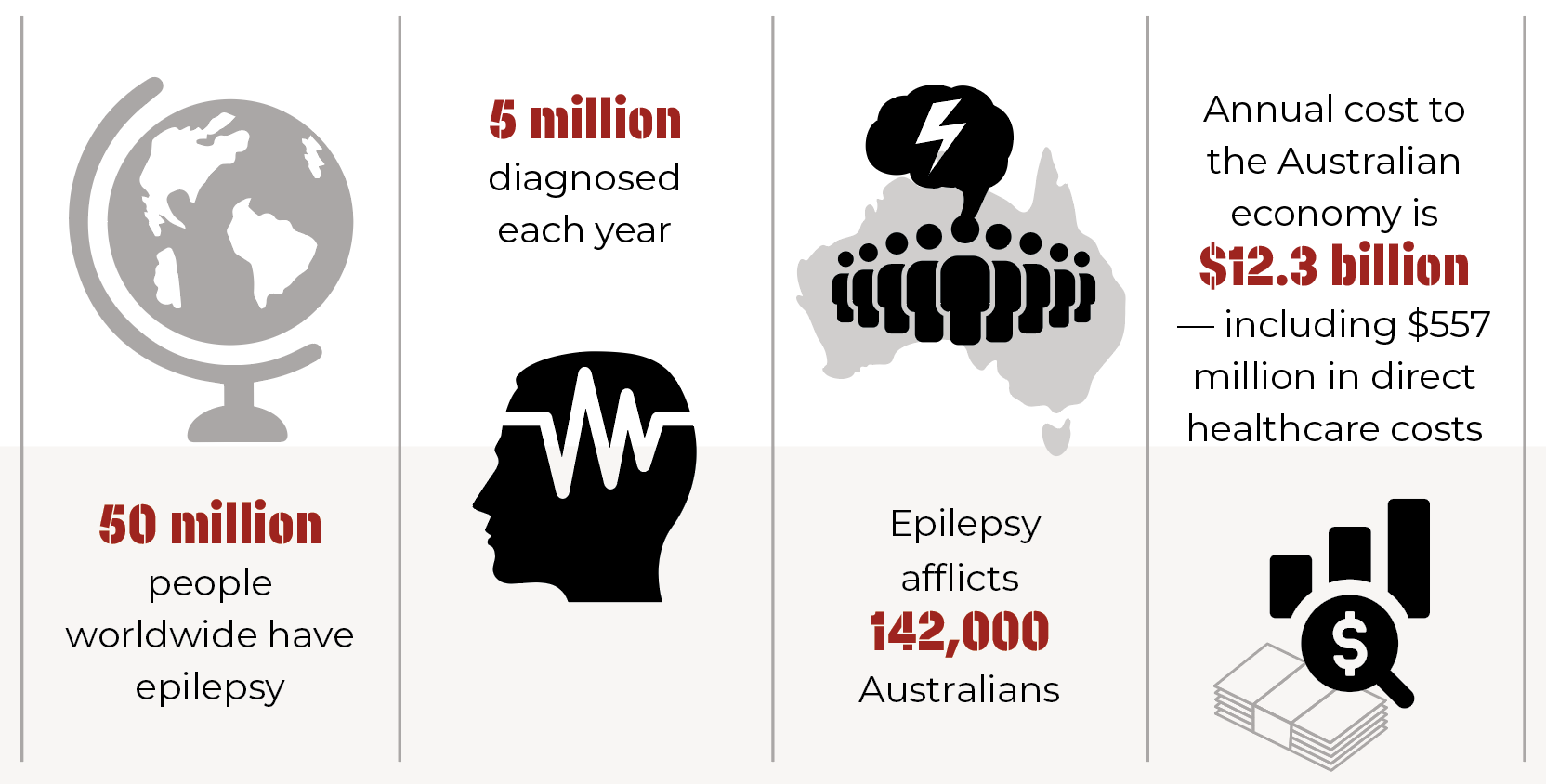
Epilepsy is a disruptive and long-term condition that afflicts more than 142,000 Australians. Characterised by seizures — the result of excessive and abnormal activity in the brain’s cortex — one of the more debilitating aspects of the condition is its unpredictability: seizures can strike at any time and without warning.
This can put sufferers of the condition in danger of physical harm, depending on what they are doing when a seizure strikes, and can limit their ability to engage in everyday activities like driving.
The unpredictability also makes diagnosing the condition difficult for doctors and unpleasant for patients.
Since epileptic seizures are characterised by an overload in neuronal activity, diagnosing them means spotting one while a patient is connected to an electroencephalogram (EEG), a device used to measure the electrophysical activity of the brain.
The problem is that this process can be awkward — and hit or miss. Best practice for diagnostic testing involves monitoring patients for five to seven days, and that has traditionally meant a hospital stay — which might not even prove conclusive.
“Some people might have an event once a year,” said George Kenley, a geomatic engineer and Chief of Strategic Projects at Australian medical device company Seer Medical.
“In traditional epilepsy monitoring, if you went into hospital, you would capture, I think, seven days, [which] equates to about 150 hours’ worth of data that someone then has to go look through in 10 second increments and go and manually eyeball.”
Seer, however, wants to make this much easier — for patients and for clinicians.
Founded in 2017 by a neurologist and two engineers, one of whom is Kenley, the company wants people who might have epilepsy to be able to stay home and undertake normal life while they’re being diagnosed. And instead of having technicians pore over troves of traced lines representing brain activity that have been drawn on pages by an EEG, Seer wants to use machine learning to help spot the signs.
That’s much more efficient than having humans search for the disruptions that might be evidence of epileptic activity too small to be visibly perceived as a seizure.
“That could take up to 40 hours in labour time costs for a neurophysiologist,” Kenley told create. “We can see more patients … whereas within the hospital setting, you’re limited by the number of resources and infrastructure that they’ve got there.“
Space to grow
But although Kenley’s work with Seer Medical is focused on epilepsy diagnostics, the first 10 years of her career were spent doing quite a different form of engineering — albeit one that would end up informing her current work in unexpected ways.
“When I was growing up, I wanted to be an architect,” she recalled. “I worked in architecture firms during uni as my work experience and I loved it, but I just saw how monotonous it was.
“Very few architects get to design anything, and then I fell into the construction side where you actually get to build, design, construct and problem-solve all in one go.”
Upon graduating, Kenley took a position at Lendlease, an opportunity she described as “a bit of luck”.
It was there that she learned how to manage large and complex projects, transforming novel-length briefs into real spaces.
A lot of these were hospitals. Kenley said there is not a direct connection between her experience building medical facilities and her current work in the biomedical domain, but it did help her develop relationships with suppliers that have proved useful.
“I think it probably allowed me to not ask as many stupid questions,” she said.

Among her accomplishments in this period of her career were the Royal Children’s Hospital Melbourne, Bendigo Hospital and Monash Children’s Hospital.
“You had to have a very close working relationship with your architects … but, in the end, us as a company would own the outcome,” she said.
“And you’d own the outcome for 25 years. So you had to be really on the ball as to what was being designed, whether it was functional, appropriate for the client, and also making sure that it was cost-effective.”
She loved the work and found the complexity rewarding.
“Prime example was I did the mental health department in the Children’s Hospital,” she said.
“Being involved with the design, we had to envisage and imagine, unfortunately, how possibly could a child get into that space and harm themselves. So it was on us as the builder to minimise that risk and take full ownership of the functionality of the space.”
Sliding Doors
Then came what Kenley calls her “Sliding Doors moment”.
She had gone on maternity leave from Lendlease for the birth of her first child. That was when an old family friend named Dean Freestone got in touch.
Freestone had spent the past 15 years researching the potential for electronics engineering to help manage epilepsy. Studying at La Trobe University and then completing his PhD at the University of Melbourne, his inquiries had also taken him to St Vincent’s Hospital in Melbourne and Columbia University in New York on a Fulbright Scholarship.
“I was fascinated with, obviously, the electricity in the body and the brain in particular,” he told create. “The way epilepsy was described to me was it was like holding a microphone too close to a speaker, like a positive feedback loop, and it required some kind of engineering style control system to be able to sort it out.”
Around 2016, Freestone decided his research had reached its limits as an academic project. To make the difference he believed was possible, he would need to commercialise the diagnostic algorithms he had been working on.
“Where you have a hypothesis that you need to test, and you’re not 100 per cent confident that it’s going to come back positive, it’s really hard to build a business around that,” he said.
“But once there’s a real feasible model around these things, that’s when a start-up model is probably more appropriate.”
Freestone developed what he calls a “loose” business plan, and then reached out to his old family friends, the Kenleys.
“When I realised that there was a commercial opportunity for us to move Seer forward, those were the first people I called,” he recalled.
“I helped Dean really closely build this business plan,” Kenley remembered. “And then I don’t think he could get rid of me.”
Freestone said Kenley took the business plan from a “D” to an “A-plus”.
“She realised the potential in what we were doing and she thought it would be a fun journey, and she was all in,” he said.
“It’s a critical piece. That sort of engineering project management mindset plugs directly into the start-up world.”
Kenley’s first task was taking the new company from a place where it was relying on research grants to one where it could attract investors.
“Gaining investment to make that first step into a commercial outcome,” Kenley said. “I just treated it as a standard project management process … I didn’t realise it would get this big, but I just bit off chunks as we went along.”
“I had a vision, and George had the ability to be able to turn that vision into something that we could actualise,” Freestone said.
The two engineers formed an effective partnership and executive team — which was rounded out by neurologist Professor Mark Cook.
“He and Dean worked very, very closely in a research relationship with Melbourne Uni and through [St Vincent’s],” Kenley said. “During the very early stages of the company, he was operationally not as involved, but, obviously as the chief medical officer, very involved in regards to medical outcomes and steering the company’s direction.”
Freestone credits Cook for creating an environment in which engineers and neurologists could collaborate effectively.
“Mark and I had worked together previously for over 10 years,” he said. “We were involved with all kinds of interesting cases at St Vincent’s Hospital, which meant that we learnt a lot about neurology and epileptology.”





Stay-at-home
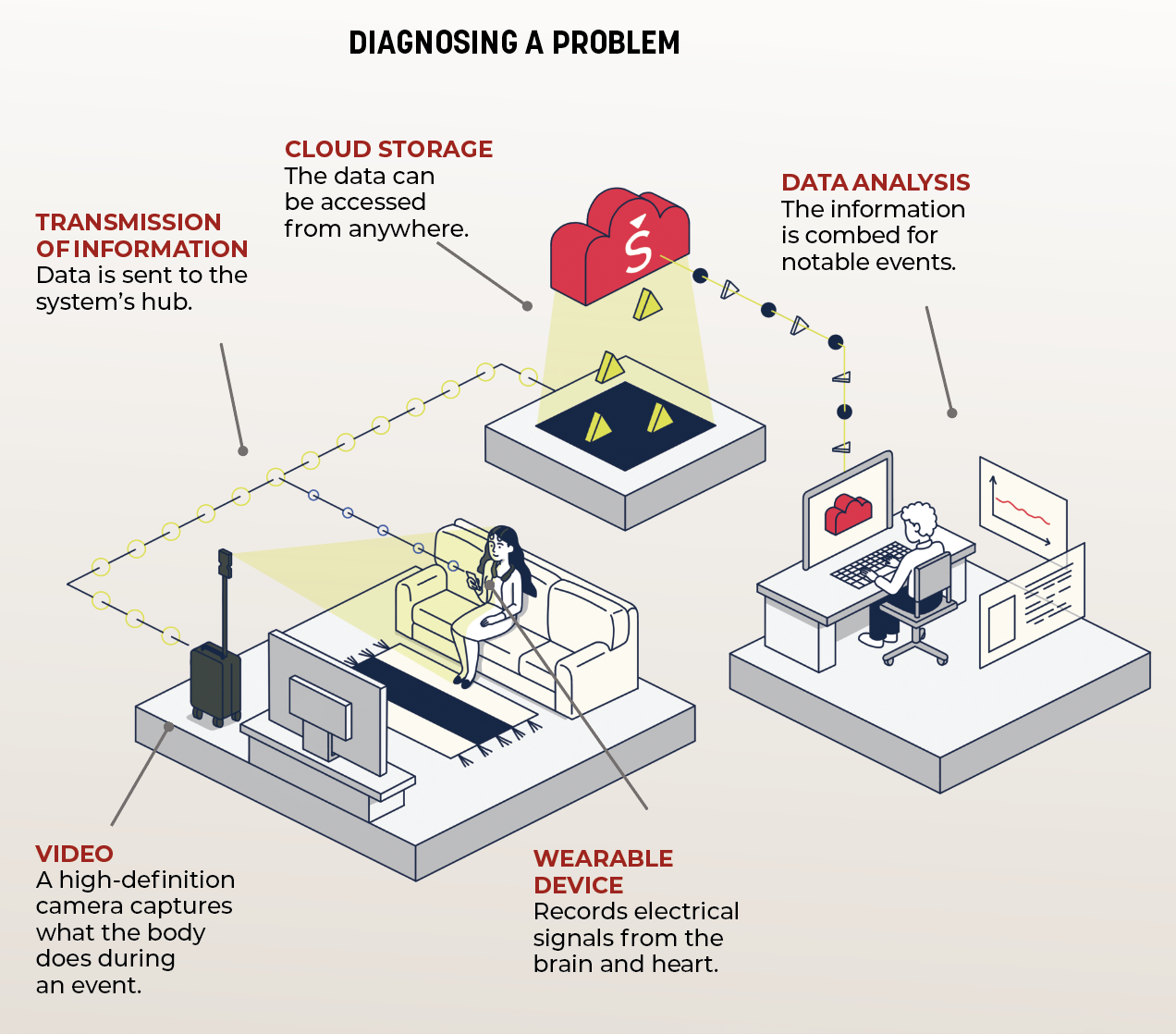
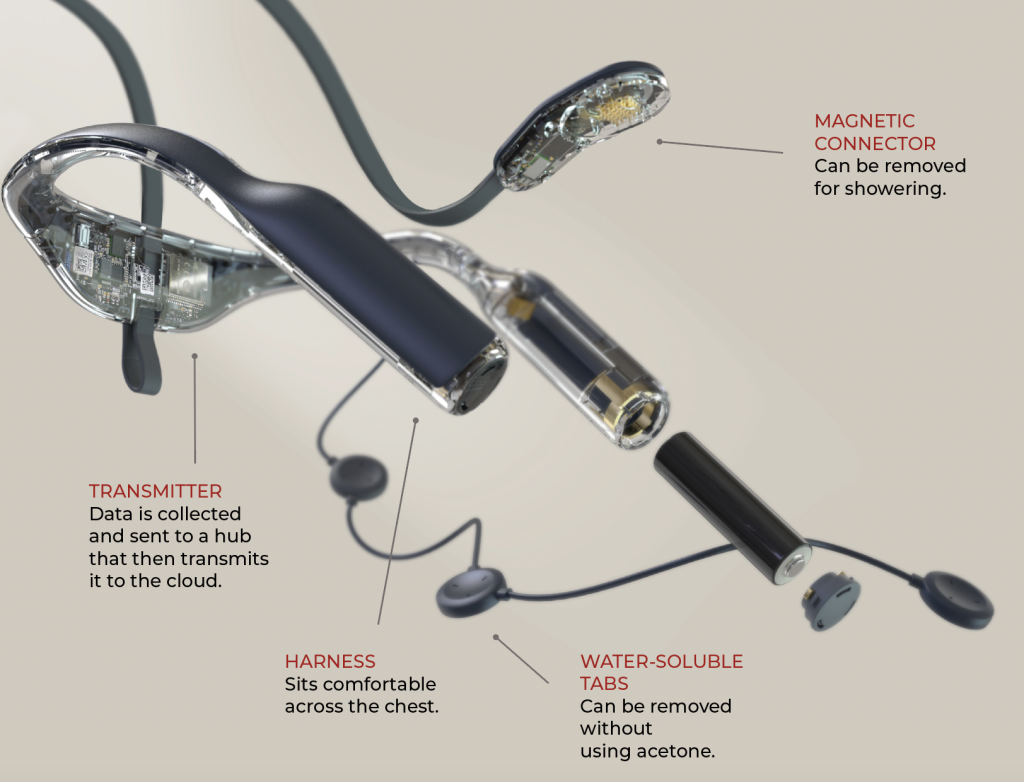
Seer’s innovation is twofold: machine learning makes identifying abnormalities in brain function quicker and easier, and the wearable Seer Sense device allows patients to be monitored at home.
Much of the ingenuity behind the device is the work of Chief Product Officer Kyle Slater. An electronics engineer, Slater came to Seer after having already worked on the bionic eye and co-founded headphone company Nura.
“Kyle is just one of the most incredible product geniuses I’ve ever met,” Freestone said. “He wants to work on problems that are big and have a global impact.”

Slater told create that producing the device first involved adapting existing systems with harnesses for at-home use.
“This taught us a lot about what worked and what didn’t,” he said. “We then took the very big step of investing in an internal team to totally redevelop the system from scratch. It was a very big undertaking, but it was the only way we could truly deliver on a step-change in experience.”
That was important because, as Kenley explained, the existing products were for use in hospitals.
“It was designed for a more sedentary patient who has to be located in their bed,” she said.
“The whole purpose behind our services is to allow patients more access, better comfort and better outcomes.”
Seer’s technology, for instance, allows patients to bathe and sleep while wearing the device. And because it uses water-soluble adhesives to gather information, patients can avoid having to be subject to harsh chemicals like acetone when it comes to removing the device.
“We’ve got some paediatric reporters at the Children’s Hospital and they’ve really found that it’s just that difference of [something as simple as] changing the electrode adhesive,” Kenley said. “You might have a kid who’s got autism or is on the spectrum, and they just get sensory overload.”
But the device doesn’t just make life more pleasant for patients — it allows more time to gather better information about their condition and improve any diagnosis.
The Seer team understands the difference this makes from firsthand experience.
“When we all started Seer back in 2017, we all got hooked up to the old system,” Kenley said. “It was terrible. I think I lasted three days.”
Taking into account comfort and wearability was a big challenge, Slater said.
“To solve this problem, we used 3D scanning and resin casting to capture the different body shapes and sizes,” he said. “We studied common contours and made a lot of prototypes we could quickly test. Material choice and composition was also a big factor.”
Seer’s ingenuity has not gone unnoticed. The device was a Gold Winner at the 2020 Good Design Awards, and was recognised this year with a gold iF Design Award.
Measuring the future
Seer’s goals for expansion currently include improving sleep studies, as well as applying the technology to cardiac diagnostics.
“To date, sleep studies have been a bit hit and miss,” Kenley explained. “You either have to spend a whole night in the hospital to get a very good kind of outcome, or you can get a dodgy, hundred-dollar job at your local chemist. So we want to improve that outpatient kind of diagnosis.”
The team also hopes to adapt its brain-monitoring technology so it can be used for the heart.
“Past that is just being able to monitor or capture really long durations of data,” Kenley said.
“Someone may have a device in either permanently or for very long periods where you can capture cyclical data across enormous lengths of time — be that months, weeks, years — and being able to provide insights out of that to give personalised insights back to a patient.”
Freestone said the technology has enormous potential.
“Epilepsy was just a beautiful starting point to then move on to all these other conditions where we can get people out of the hospital into the home environment,” Freestone said.
“We believe we stand a fairly big chance of being the next big medtech company in Australia … that would be synonymous with ResMed and Cochlear. The opportunity is certainly there, and we plan to take it.”